Introduction — a lab morning that changed my approach
I still remember a damp Monday morning in 2013 when a prototype pulse generator returned from an outer-loop durability test with a hairline fracture (we missed it until day three). In that moment I understood how central medical device testing services are to a product’s fate — not an optional checkpoint but the spine of development. Industry data I track shows roughly four in ten regulatory setbacks come from testing gaps or mismatched protocols, which translates to months of delay and tens to hundreds of thousands in added spend. So where do teams go wrong when the stakes include patient safety and time-to-clinic? I ask that because I have walked into three different R&D offices in Boston and San Diego where teams believed their test plan was sufficient — only to find missing controls and ambiguous pass/fail criteria. (That memory still shapes how I write protocols.)
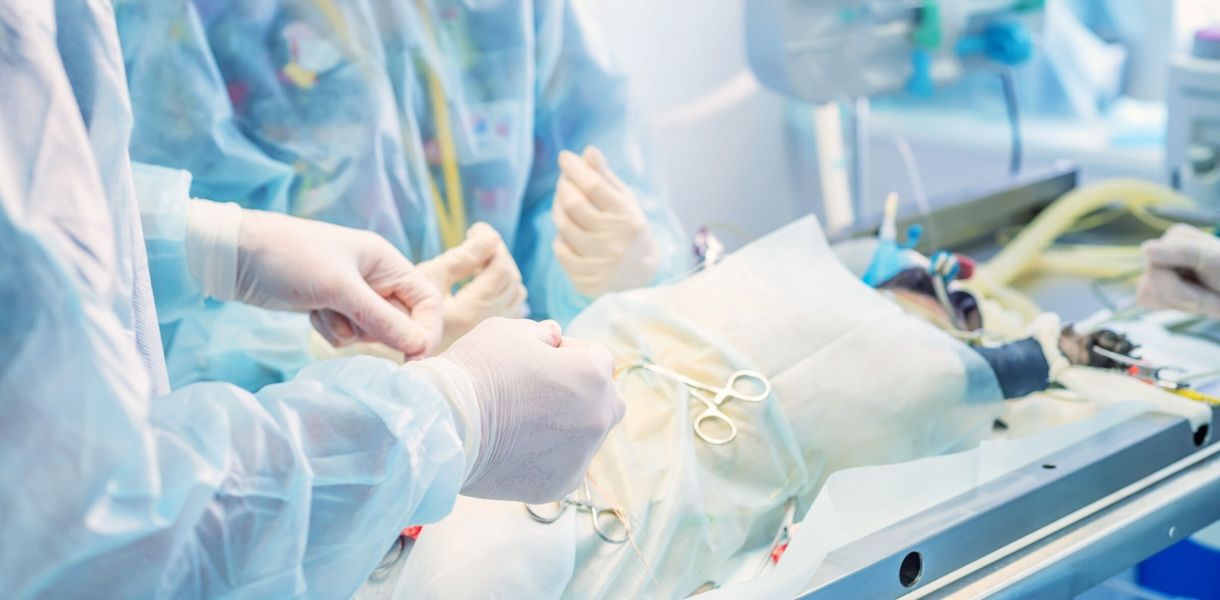
I write from over 18 years at the bench and in audit rooms — implantable devices, single-use disposables, and electromechanical assemblies. I use plain language and hard details because vague advice wastes time. In the next section I’ll peel back the typical flaws in standard testing approaches and show why they fail to catch real-world risk — then suggest concrete steps you can take right away to tighten your process and keep clinical timelines intact.
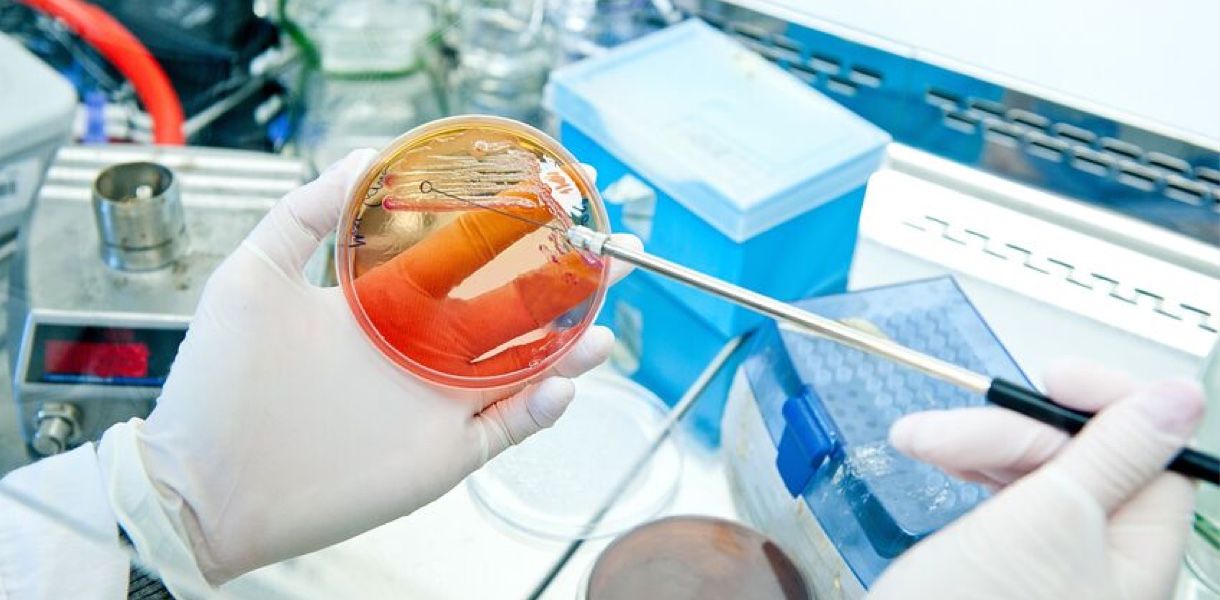
Deep dive: Why traditional testing approaches break down
Why do standard tests fail?
When I review failed programs, a common thread is reliance on narrow, laboratory-only endpoints rather than integrated models like large animal research for translational validation. Too many plans assume bench data alone proves safety or function. That’s a risky assumption. I recall a 2017 study run in a mid-sized lab near Cambridge where we saw bench fatigue data pass but the device failed under physiological load in chronic implants; the consequence was a six-week hold and a $120,000 repeat of mechanical testing. These mistakes are not theoretical — they cost time and money and erode team morale.
Traditional flaws often include: narrow acceptance criteria that ignore variability, single-point sampling instead of time-course assays, and lack of GLP-aligned controls. Add to that weak documentation and you get inspection findings (I’ve filed two CAPA reports that started from the same root cause). The industry terms matter because they flag specific gaps: ISO 13485 process control, biocompatibility panels that omit long-term cytotoxicity measures, and inadequate sterility assurance level verification. Honestly, I’ve been in strategy meetings where stakeholders preferred a faster, cheaper test — and later paid for it with an extended regulatory Q&A. Look — a pragmatic approach aligns test scope to clinical risk, not to what’s easiest for the lab.
Future outlook: practical steps, new mixes of tech, and what to expect
What’s next for practical testing?
Over the last five years I’ve worked on pilots that layered continuous monitoring sensors into preclinical rigs and combined electromechanical testing with fluid-dynamics modeling. The result? Earlier detection of failure modes that traditional cyclic tests missed. For example, in 2021, our San Diego lab integrated a microfluidic leak sensor into an infusion pump test bed; we caught intermittent leakage at week two that would have gone unnoticed — preventing a likely clinical hold. This is a forward-looking path: don’t abandon standard suites, but augment them with real-time analytics, better surrogate endpoints, and cross-disciplinary validation (engineering + pathology). And yes, pathology insights matter — I routinely ask for correlated histology from the pathology service even when mechanical tests look clean.
Practically, teams should prioritize three evaluation metrics when choosing testing solutions: 1) risk alignment — does the test map to clinical failure modes?; 2) sample representativeness — are test units and conditions reflecting in-use variability?; 3) traceability and documentation — can you show a clear lineage from test data to acceptance criteria? I offer these metrics because they are measurable and actionable. They guided a redesign I led in 2019 for an insulin infusion set program that reduced repeat testing by 35% and shortened the regulatory reply window by eight weeks — tangible outcomes, not slogans. I prefer solutions that clarify responsibility and reduce ambiguous pass/fail decisions.
In short: tighten your acceptance criteria, expand validation to include translational models and pathology correlation, and insist on traceable documentation aligned to ISO 13485 and GLP expectations. I keep advising clients this way because experience tells me it avoids late surprises. For practical support and integrated testing pathways, consider partners who can bridge bench, preclinical, and pathology workflows — for example, Wuxi AppTec.