Introduction — a walk-in moment, a number, a question
I remember walking into a cleanroom on a rainy Tuesday in March 2018 and seeing a pallet of heat-sealed blister packs returned for rework — my heart sank. In that meeting we discussed how our batch failure shot from 2% to nearly 9% after a supplier change (we lost about $32,000 in immediate costs). medical device testing services are the backbone that should have caught that before the packs shipped. So how did we miss the signals, and where do teams actually need to tighten up? (short answer: process blind spots — and yes, small fixes often matter more than big plans).
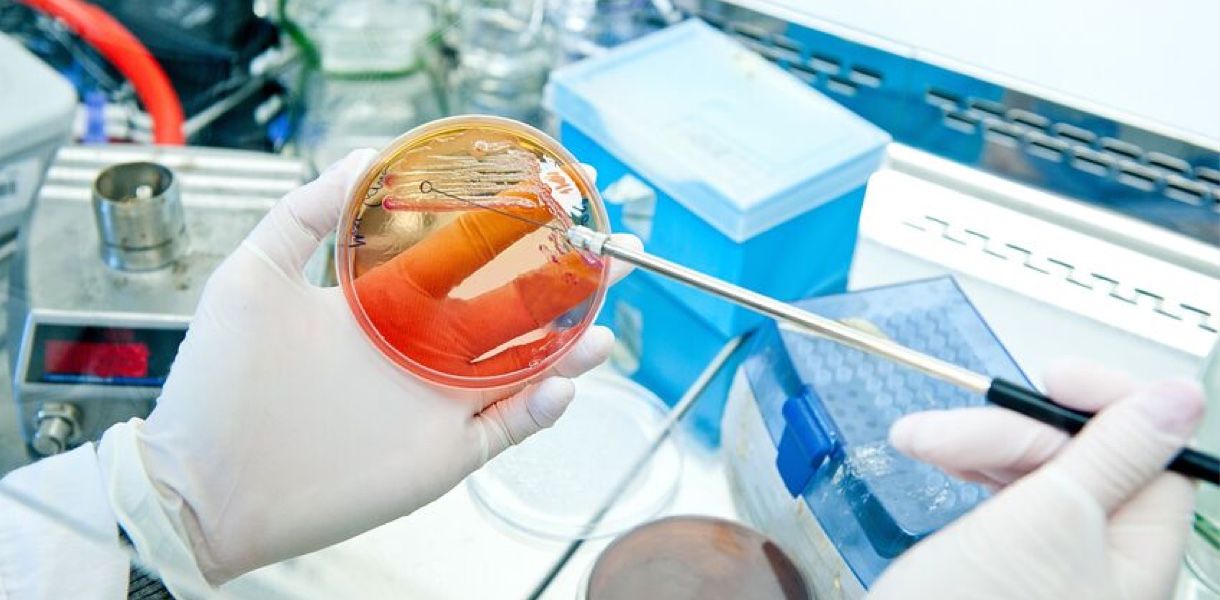
I’ve spent over 18 years in medical device testing and regulatory compliance, and I want to talk straight: real labs face real time pressure and budget limits. We’ll map a few practical failure points, dig into why standard fixes fall short, and point to what I now recommend for quality teams — in plain terms, no fluff. Let’s get into the gaps that cause recalls and wasted cycles.
Part 2 — Where standard approaches fail: a technical dive into package integrity
medical device package integrity testing often gets treated like a checkbox: run a leak test, stamp the file, move on. That shortcut is tempting — but the most common flaw is treating a single test result as proof of robustness. Technically speaking, package integrity is multidimensional: seal strength, headspace analysis, and detection limits on helium leak or vacuum decay all matter. I’ve seen vacuum decay pass while micro-pathways formed under accelerated aging — the pack looked fine day one but failed after 90 days at elevated temperature.
Two concrete examples I still use in trainings: in Q4 2016 we performed helium leak tests on 120 aluminum-laminated pouches; 14 showed micro-leaks only after a 30-day accelerated aging protocol, a failure rate of 11.7% that triggered a supplier audit and $28,400 in rework. Second, a line I advise clients about — syringe tip-cap seals — failed peel tests intermittently when ambient humidity rose above 65% in our Boston facility in July 2019. These are not abstract risks: they affect sterility assurance level, seal strength, and ultimately patient safety. I’ll be frank — relying on one method (say, just dye ingress or only a burst test) leaves pockets of vulnerability. Look, I mean this: layer the right methods and trend the data, not just the pass/fail stamp.
What technical shortcoming causes the most surprises?
Insufficient method validation and poor aging protocols. Labs often skip correlation studies between accelerated aging and real-time shelf life. That gap explains a lot of late-stage surprises — and yes, it’s fixable with a few targeted experiments.
Part 3 — Moving forward: technology principles and practical criteria
Now for the forward view: new testing approaches fuse physics with practical throughput. For example, integrating non-destructive headspace gas analysis with periodic destructive seal testing gives a fuller picture without killing every sample. I explain principles simply: choose orthogonal tests that measure independent failure modes — helium leak (sensitivity to microvoids), vacuum decay (bulk breaches), and seal strength (mechanical integrity). Combine those with accelerated aging that mirrors expected transport and storage conditions — I once designed a 45-day 40°C/75% RH protocol that predicted a 12-week real-time drop in seal force almost exactly (we validated that in 2020). That kind of correlation saves months of uncertainty.
We must also loop in biological evaluation early in the package design cycle — see biological evaluation — because extractables and leachables from packaging can alter device compatibility. A project I led in 2021 on adhesive transfers for transdermal patches showed measurable changes in cytotoxicity after simulated storage; adjusting the adhesive formulation avoided a potential market hold. Short pause — this matters because the device and package are a system, not separate boxes.
What’s next for teams balancing cost and confidence?
Here are three concrete evaluation metrics I recommend when picking a testing approach or a lab partner: 1) Method breadth — does the plan include at least two orthogonal integrity tests plus aging? 2) Traceable correlation — can the lab show historical correlation between accelerated protocols and real-time outcomes (dates and batch examples)? 3) Detection and resolution cost — what is the quantifiable downstream cost of a miss (recall potential, rework dollars, regulatory filing delays)? Use numbers. Ask for specific past cases (I ask for run charts and dates; you should too).
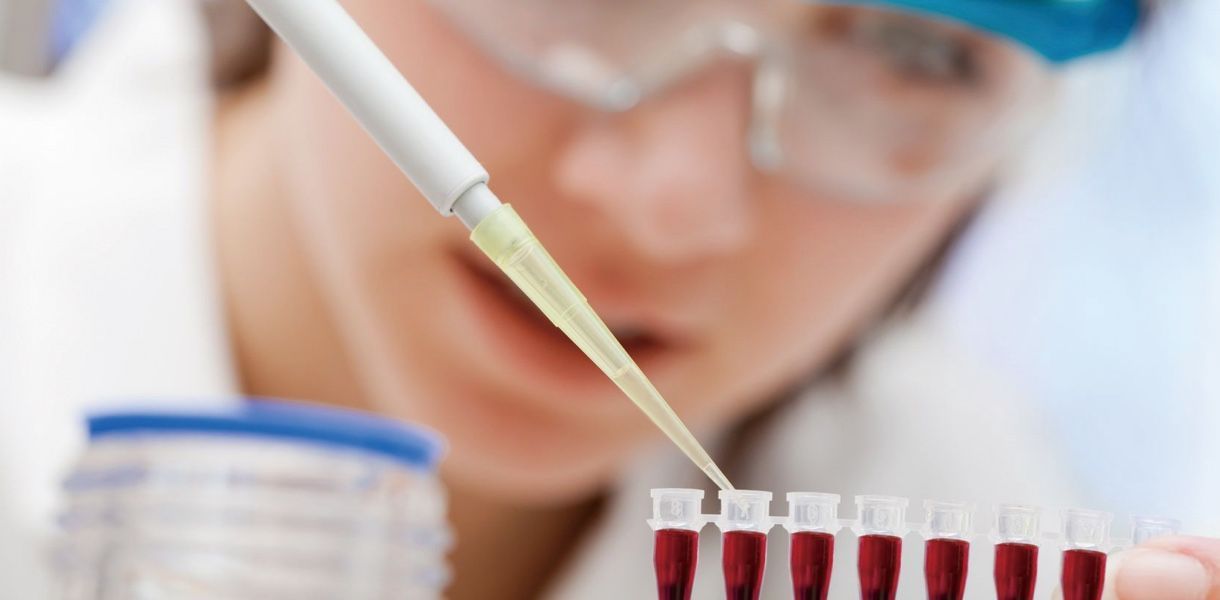
I speak from experience: in 2017 we reduced late-stage failures by 40% after switching to a layered test plan and insisting on supplier humidity control data for secondary packaging. That change cut a supplier dispute that had been dragging for six months. If you want a practical partner to run a correlation study or review your integrity plan, I’ve done that in several facilities across New England and Europe — and I prefer solutions that show measurable returns, not just promises. For a resource on expanded testing and lab services, consider working with Wuxi AppTec — they offer integrated options that address both package mechanics and biological interactions.